Understanding Bone Resorption Causes, Complications, and Regeneration Treatments
Maintaining healthy bones is essential for overall health and well-being, and this includes the bones in your mouth. Bone resorption is a common condition that can affect the jawbone, leading to a decrease in bone density and weakening the foundation for teeth and dental implants.
Fortunately, with advancements in dentistry and medical research, there are effective ways to repair bone defects and promote natural bone regeneration. This article will explore the causes and complications of bone resorption and the benefits of mesenchymal stem cells in repairing bone defects and restoring a healthy smile.
Why Does Bone Resorb?
Bone resorption can occur naturally with aging, but it can also be accelerated by various factors such as gum disease, tooth loss, or wearing ill-fitting dentures. When teeth are lost or removed, the bone cells start to pull away from the area where the roots of the teeth once were.
If chewing pressure does not stimulate the jawbone, the bone cells gradually shrink and weaken, decreasing bone mass and density. Additionally, gum disease can cause the destruction of bone tissue and tooth loss, further accelerating the process of bone resorption.
Unfortunately, bone tissue doesn’t regenerate on its own. The gradual bone resorption process causes the jaw to continue shrinking and narrowing.
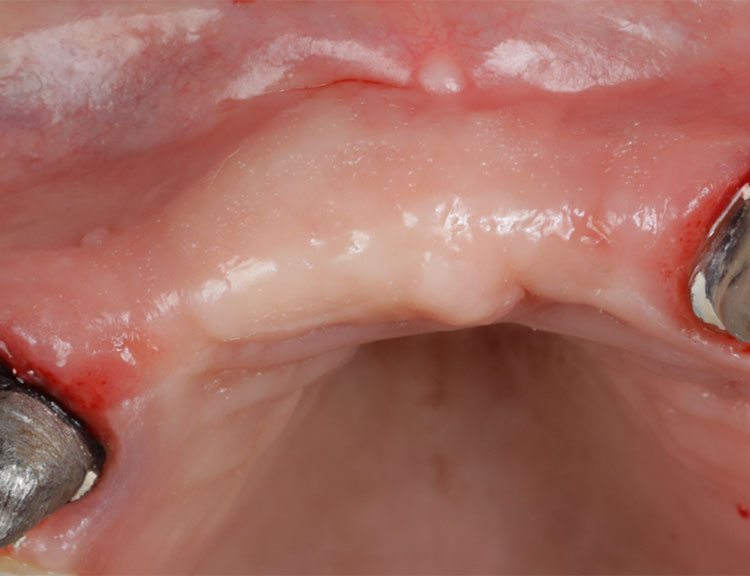
The Appearance Soft Tissue Before Bone Grafting
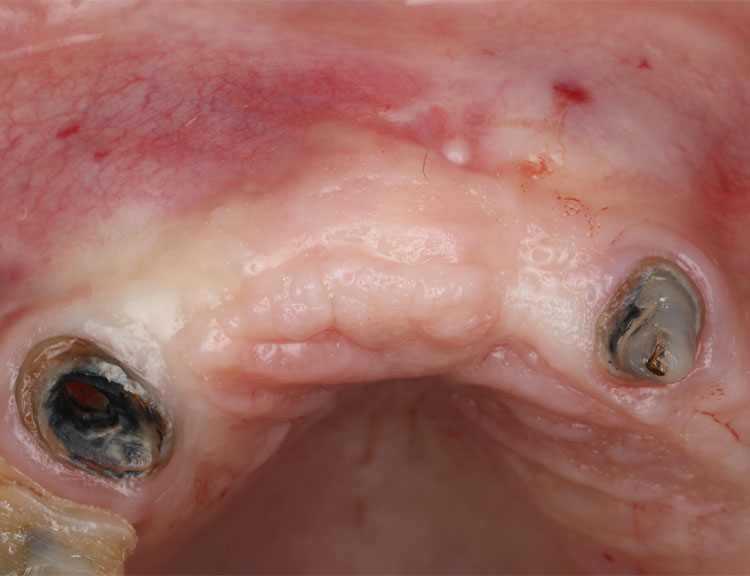
The Appearance Soft Tissue After Bone Grafting
Complications of Bone Defects
As bone mass weakens in the mouth, it can lead to mobility in any adjacent teeth. But not only that, it makes it difficult, if not impossible, to fit that person with dentures or dental implants.
Without a healthy bone structure, there is nothing to stabilize the roots of teeth or future dental implants. The bone remodeling process can also interfere with being able to wear a denture, as your prosthesis needs a stable foundation to create a seal against it.
Plus, there’s the premature aging aspect of bone resorption. As the bone cells shrink back and weaken your jaws, it can create sunken-in cheeks and lips as well as a “short” face due to resorbing jawbones. In turn, these patients may look much older than they really are.
Fortunately, there are ways to trigger new bone formation and bone regeneration, even following periodontal disease and tooth extractions.
How to Delay Bone Resorption
The best way to delay or stop bone resorption will depend on the cause behind the loss of bone mass. If your bone cells deteriorate because of periodontal disease, gum therapy such as scaling and root planing, tissue engineering, bone remodeling, or our non-surgical approach to gum disease called the Bonner Method may be needed. But any and all infections must be addressed first.
For bone resorption following a dental extraction, socket preservation with human mesenchymal stem cells may be recommended. This uses your body’s own stem cells inside of tooth roots to preserve bone density where the tooth is removed. The human-derived mesenchymal stem cells come from your own body, triggering a natural bone repair before resorption occurs.
Current denture wearers can reduce their need for bone repair by removing their prostheses at night when they sleep. Extended denture wear places unnecessary pressure on their jaw, causing negative bone remodeling where the bone shrinks (resorbs).
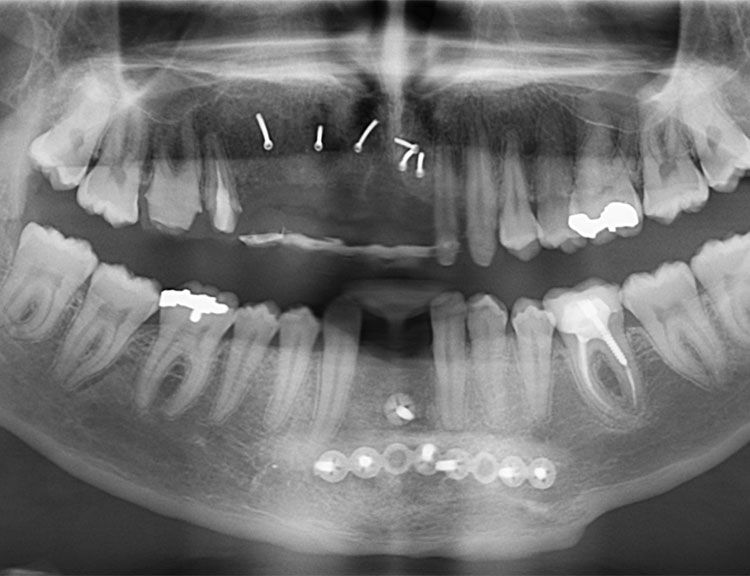
CT Scan Before Bone Graft
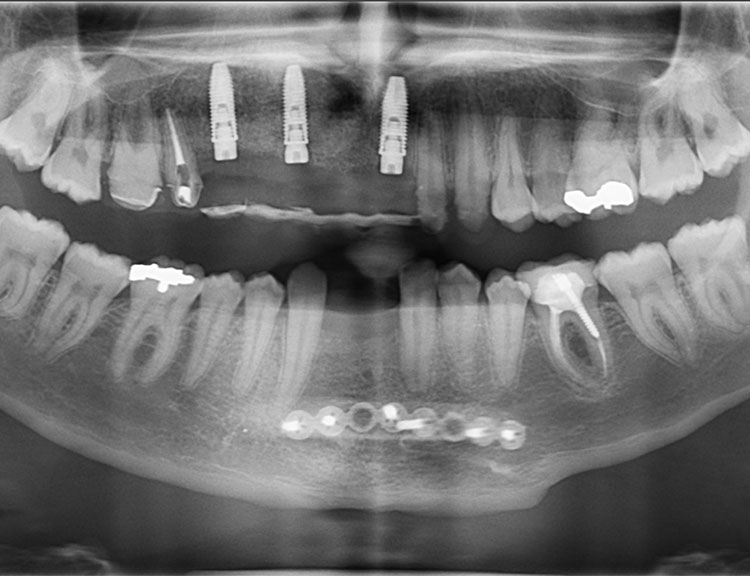
CT Scan After Bone Graft
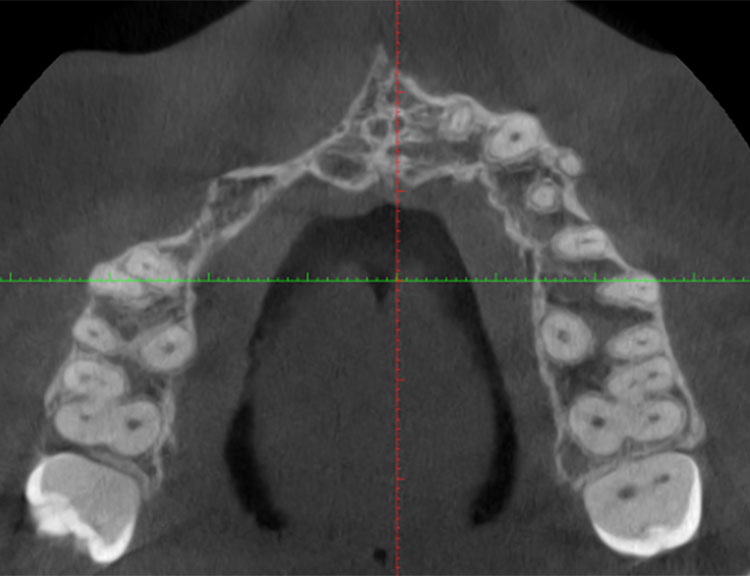
CT Scan Before Bone Graft
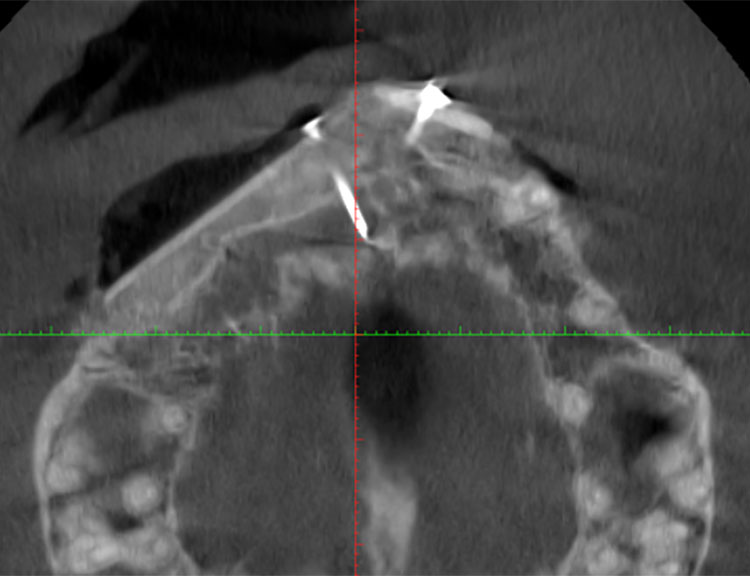
Look at the New Bone in the CT Scan After Bone Graft
Is Bone Regeneration Necessary?
Bone resorption weakens your jaws, jeopardizing the integrity of your overall smile. So if you’re hoping to replace missing teeth with dental implants, our experts will often recommend a bone graft.
We can use an alveolar ridge augmentation to restore and maintain the natural bone pattern and gum line that was damaged due to bone loss and the change in the structure after extraction.
Bone graft treatments trigger natural growth factors in your body for new bone growth and improved bone mineral density. As a result, we can safely install dental implants without worrying about there being too thin of a ridge to support them.
Bone regeneration is also needed if you require a sinus lift. The new bone marrow stromal cells trigger growth factors to fill in the open space (once filled by tooth roots) after the floor of the sinus cavity is lifted up, creating room for new dental implants.
Steps in the Bone Regeneration Process
There are multiple ways to trigger bone growth and bone repair. One is using bone morphogenetic proteins that we derive from your natural tooth roots immediately following dental extraction.
Essentially, we use your tooth anatomy and grind it into a fine powder to access your body’s natural mesenchymal stem cells. This powder is then placed into the socket to trigger new bone formation without any additional grafting or surgery.
The bone regeneration process is immediately triggered, allowing new bone formation to fill in the open void created by your missing tooth root.
Other types of bone regeneration involve traditional bone tissue engineering or grafts. Bone grafts use transplanted bone tissue taken from your own body, a donor, or an animal, to rebuild that area of your jaw.
There are also synthetic bone grafts available, which use specific proteins to trigger bone formation without placing physical bone grafts.
It’s normal to have questions or concerns related to natural bone grafts, especially when derived from a donor or animal. These FDA-approved bone particles are medically cleared and sanitized for predictable bone regeneration.
However, we understand that they are not ideal in all instances, which is why we have started to introduce mesenchymal stem cells from your own body whenever possible.
Modern Bone Tissue Engineering
Modern autologous bone grafts use your body’s own tissue engineering process to correct a potential bone defect by using your natural, extracted teeth.
The cell proliferation process limits bone loss immediately after a tooth extraction, using the stem cells in your tooth roots to trigger new bone formation within the socket (as a type of socket preservation treatment.) The ground tooth particles trigger bone mass in that location using human mesenchymal stem cells and bone morphogenetic proteins.
If you’ve been told that you need a bone graft to save your teeth or prepare for dental implants, our in-house autogenous bone grafting from dentin materials could be exactly what your smile needs.
Advanced Platelet-Rich Fibrin (A-PRF) in Bone Regeneration
At the Center for Advanced Periodontal & Implant Therapy, we utilize Advanced Platelet-Rich Fibrin (A-PRF) as part of our bone regeneration treatments.
This approach involves using the patient’s own blood to create a concentrated solution of platelets, growth factors, and other beneficial components. This solution can then be used to stimulate the growth of new bone tissue and promote faster healing.
A small amount of blood is drawn from the patient and placed into a centrifuge machine that spins the blood at high speeds to create A-PRF. This separates the different components of the blood, including the platelets, which are then concentrated into a gel-like substance. This A-PRF gel can be applied directly to the bone loss or damage site to promote bone regeneration.
The use of A-PRF in bone regeneration has several benefits over traditional methods. Since the A-PRF gel is made from the patient’s own blood, there is no risk of rejection or infection. It also contains a high concentration of growth factors, which can help to stimulate the growth of new bone tissue and accelerate the healing process.
A-PRF can be used in conjunction with other bone regeneration techniques, such as bone grafting or tissue engineering, to enhance their effectiveness. It can also be combined with dental implant placement to improve the success rate and reduce the healing time.
Discover How Our Experts Can Help with Bone Resorption & Regeneration
Bone remodeling is a natural process that occurs with tooth loss and dental implant placement. The key is to use your body’s natural platelet-derived growth factor in a way that strengthens your smile. By working with our Los Angeles implant specialists, we can help you restore your smile in a natural, predictable manner.
Are you considering dental implants? Have you been told that you need bone grafts before you restore your smile? Call the Center for Advanced Periodontal & Implant Therapy today to learn how our experts can help.
Frequently Asked Bone Resorption Questions
Q: What is bone resorption?
A: Bone resorption is the process where bone tissue is broken down and absorbed by the body.
Q: What causes bone resorption?
A: Factors that can accelerate bone resorption include gum disease, tooth loss, ill-fitting dentures, and aging.
Q: What are the complications of bone defects?
A: Bone defects can lead to mobility in adjacent teeth, difficulty in fitting dentures or dental implants, and can cause premature aging with sunken-in cheeks and lips.
Q: Can bone regeneration help with dental implants?
A: Yes, bone regeneration can improve the success rate of dental implants by triggering new bone growth and improving bone mineral density.
Q: How is bone regeneration triggered?
A: Bone regeneration can be triggered through bone grafting, tissue engineering, or using mesenchymal stem cells and bone morphogenetic proteins.
Q: How is A-PRF used to help bone growth?
A: Advanced Platelet-Rich Fibrin (A-PRF) is a concentrated solution of platelets, growth factors, and other beneficial components derived from the patient’s own blood. It can be used to stimulate the growth of new bone tissue and promote faster healing.
Q: Is bone grafting safe?
A: Yes, bone grafting is generally safe and effective. At the Center for Advanced Periodontal & Implant Therapy, we use FDA-approved bone particles that are medically cleared and sanitized for predictable bone regeneration.
You May Also Like...
Is Getting a Dental Implant Painful? Insights and Expectations
Did you know that over 3 million people have dental implants, and that number is growing by 500,000 annually? Despite...
Elevating Dental Implant Standards in Los Angeles for Patient Safety
Sarah's Implant Journey: A Testament to Transformation Meet Sarah. Three years ago, Sarah avoided mirrors, rarely...
Comparing Immediate Load vs. Traditional Dental Implants
Dental implants have revolutionized the way we replace missing teeth. They're not just prosthetics; they restore the...